Symantec DLP Used to Protect BAS Systems
- BAS
- 27.09.2012
- MyEnroll360 Security
BAS takes the privacy and security of its clients' information very seriously. Toward that end, BAS utilizes state of the art security and virus protection software. In ...
READ MORE
Symantec DLP Used to Protect BAS Systems
- BAS
- 27.09.2012
- MyEnroll360 Security
BAS takes the privacy and security of its clients' information very seriously. Toward that end, BAS utilizes state of the art security and virus protection software. In ...
READ MORE
Easy and Efficient Open Enrollment through MyEnroll.com
- BAS
- 27.09.2012
- MyEnroll360 Feature
BAS works closely with employers to prepare for open enrollment. Online enrollment through BAS' MyEnroll.com allows employees to easily and quickly select benefits ...
READ MORE
COBRA Disability Extension
Q.- A COBRA continuant requested an extension of coverage due to disability. The continuant provided a copy of the Social Security Administration's disability award. ...
READ MORE
Wellness Program's ADA Implications
- BAS
- 27.09.2012
- HR & Benefits Compliance
The U.S. Court of Appeals for the 11th Circuit recently held in Seff v. Broward County that a wellness program complied with the Americans with Disability Act (ADA) safe ...
READ MORE
Individual Mandate May Have an Unintended Impact
- BAS
- 27.09.2012
- Health Care Reform (ACA)
Health care reform's individual mandate requires most Americans to maintain minimum essential health insurance coverage. Beginning in 2014, individuals who do not comply ...
READ MORE
Qualified Transportation Benefits
- BAS
- 19.09.2012
- HR & Benefits Compliance
Many employers, particularly employers in urban locations, provide qualified transportation benefits to their employees. A Qualified Transportation Plan is offered under ...
READ MORE
Guidance on 90 Day Waiting Period Limitation Under Health Care Reform
- BAS
- 19.09.2012
- Health Care Reform (ACA)
The Affordable Care Act provides that for plan years beginning on or after January 1, 2014, a health plan cannot apply any waiting period that lasts more than 90 days. A ...
READ MORE
Question of the Week
Q.- We offer employees the opportunity to participate in a health flexible spending account plan. We contribute $3,000 to each employee's FSA. I know there are new ...
READ MORE
Unencrypted Laptop Theft Leads to $1.5 Million HHS Settlement
- BAS
- 19.09.2012
- MyEnroll360 Security
The U.S. Department of Health and Human Services (HHS) announced a $1.5 million settlement with Massachusetts Eye and Ear Infirmary (“MEEI”). The settlement is a result ...
READ MORE
Unencrypted Laptop Theft Leads to $1.5 Million HHS Settlement
- BAS
- 19.09.2012
- MyEnroll360 Security
The U.S. Department of Health and Human Services (HHS) announced a $1.5 million settlement with Massachusetts Eye and Ear Infirmary (“MEEI”). The settlement is a result ...
READ MORE
In/Out Board on MyEnroll Creates Central Location for Team ...
- BAS
- 19.09.2012
- MyEnroll360 Feature
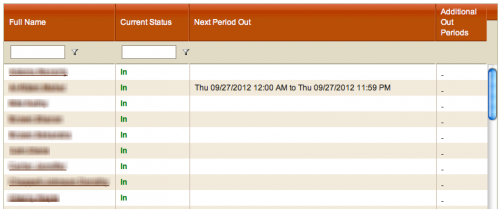
The In/Out Board on MyEnroll.com can provide a central location for your HR team to coordinate vacation, telecommuting, and training schedules to ensure sufficient ...
READ MORE
Determining Full-Time Employees for Pay-or-Play Penalty
- BAS
- 13.09.2012
- Health Care Reform (ACA)
Beginning 2014, certain employers must offer their employees appropriate health coverage or be subject to a tax penalty. See our article dated July 5, 2012. This "pay or ...
READ MORE
Telemedicine – A New Enhancement to Employee Benefits
- BAS
- 13.09.2012
- HR & Benefits Compliance
Telemedicine is a relatively new health care concept that is a desired enhancement to many health plans. According to the American Telemedicine Association, ...
READ MORE
Question of the Week - Change in DCAP Election for Spouse's Work ...
Q.- We have an employee who wants to change her Dependent Day Care Flexible Spending Account Plan contribution amount because her spouse has switched from full-time to ...
READ MORE
Cobra Control Services, LLC Provides Automated COBRA Administration
- BAS
- 12.09.2012
- MyEnroll360 Feature
BAS' COBRA administration service through its subsidiary Cobra Control Services, LLC provides a full-service COBRA administration alternative. Our automated process ...
READ MORE
Cobra Control Services, LLC Provides Automated COBRA Administration
- BAS
- 12.09.2012
- MyEnroll360 Feature
BAS' COBRA administration service through its subsidiary Cobra Control Services, LLC provides a full-service COBRA administration alternative. Our automated process ...
READ MORE
Approved Software List
- BAS
- 12.09.2012
- MyEnroll360 Security
Employers may benefit from implementing procedures to address software employees download to company computers for both personal and business use. Monitoring software on ...
READ MORE
Approved Software List
- BAS
- 12.09.2012
- MyEnroll360 Security
Employers may benefit from implementing procedures to address software employees download to company computers for both personal and business use. Monitoring software on ...
READ MORE
Question of the Week - HIPAA Applicability to FMLA Documentation
Q.- One of our employees has requested FMLA leave and has provided a lot of documentation from her doctor about her medical condition. Do I have to be concerned with ...
READ MORE
Religious Exemption for Women's Contraceptive Coverage
- BAS
- 06.09.2012
- Health Care Reform (ACA)
The Affordable Care Act requires non-grandfathered health plans to provide coverage for preventive care services without cost-sharing. Some preventive care services ...
READ MORE
Consider Disability Issues when Implementing Technology Changes
- BAS
- 06.09.2012
- HR & Benefits Compliance
The Department of Labor recently posted a blog entry reminding employers to consider disability discrimination issues when implementing technology in the workplace.
READ MORE
How to Correct a Denied Flexible Spending Account/Health ...
- BAS
- 06.09.2012
- MyEnroll360 Feature
Each week, BAS receives more than 2,500 flexible spending account and/or health reimbursement account claims. Approximately 85% of claims submitted to BAS are properly ...
READ MORE
Flexible Spending Account/Health Reimbursement Account Denied Claims
- BAS
- 06.09.2012
- MyEnroll360 Feature
Each week, BAS receives more than 2,500 flexible spending account and/or health reimbursement account claims. Approximately 85% of claims submitted to BAS are properly ...
READ MORE
NIST Offers Risk Assessment Toolkit for HIPAA Security Rule Analysis
- BAS
- 06.09.2012
- MyEnroll360 Security
The Security Rule of the Health Insurance Portability and Accountability Act (HIPAA) established national standards to protect individuals’ electronic personal health ...
READ MORE
NIST Offers Risk Assessment Toolkit for HIPAA Security Rule Analysis
- BAS
- 06.09.2012
- MyEnroll360 Security
The Security Rule of the Health Insurance Portability and Accountability Act (HIPAA) established national standards to protect individuals’ electronic personal health ...
READ MORE
About BAS' Newsletter
Join our free, weekly blog email list to be the first to learn about the hottest HR Issues, MyEnroll360 Features, Systems Security, and Weekly Topics of Interest.
"The News to Use that BAS/CCS sends every Thursday always has great info, but particularly the Question of the Week is a great resource!"

Account Manager / Employee Benefits
PA Insurance Broker
PA Insurance Broker
Recent Posts
Posts by Topic
- HR & Benefits News (615)
- MyEnroll360 Security (555)
- MyEnroll360 Feature (539)
- Health Care Reform (ACA) (536)
- HR & Benefits Compliance (526)
- HR & Benefit Plans (468)
- Technology News (326)
- MyEnroll360 News (274)
- Affordable Care Act (265)
- MyEnroll360 (264)
- COBRA (173)
- Company News (152)
- HR & Benefits (148)
- BAS News (126)
- Affordable Care Act (ACA) (99)
- Cybersecurity (87)
- Healthcare FSA (83)
- COBRA Administration (77)
- Dependent Day Care FSA (72)
- Covid (65)
- Flexible Spending Accounts (64)
- COBRA Premium Billing (52)
- MyEnroll360 Capabilities (50)
- Eligibility & Enrollment (41)
- MyEnroll360 Application (39)
- MyEnroll360 Solutions (39)
- coronavirus resources (27)
- Health Care Flexible Spending Account (HCFSA) (20)
- HIPAA (17)
- Medicare (17)
- Benefits Administration (15)
- Taxes (15)
- Compliance (14)
- Health Care Exchanges (12)
- Health Reimbursement Accounts (12)
- Enrollment/Eligibility (11)
- Leave Premium Billing (11)
- Wellness Programs (11)
- BAS Solutions (10)
- Enrollment & Eligibility (10)
- Location Premium Billing (10)
- BAS Services (8)
- Human Resources Administration (8)
- Payroll (8)
- Retiree Premium Billing (8)
- IRS (7)
- Enrollment (6)
- Premium Billing (6)
- health insurance coverage (6)
- Dependent Audit (5)
- Direct Premium Billing (5)
- EDI (5)
- HSA (5)
- Open Enrollment (5)
- Question of the Week (5)
- Retire Premium Billing (5)
- SHOP Exchange (5)
- Business Growth (4)
- Cost Savings (4)
- Location Premium & Expense Billing (4)
- MyEnroll360 Operations (4)
- healthcare resources (4)
- Applicable Large Employers (ALEs) (3)
- Conferences (3)
- Data Collection (3)
- Dependent Verification (3)
- Equal Employment Opportunity Commission (EEOC) (3)
- U.S. Department of Labor (3)
- Affordability Percentage for Health Coverage (2)
- Brokers and Consultants (2)
- EEO-1 Data (2)
- Life Event Manager (2)
- Mass Email Manager (2)
- Medical Plan (2)
- Multi-Factor Authentication (MFA) (2)
- New Hire (2)
- PCORI Fee (2)
- Pension (2)
- Phishing Emails (2)
- Solutions (2)
- 125 Plans (1)
- Benefits.gov (1)
- CHIP Notice (1)
- Cafeteria Plans (1)
- Children's Health Insurance Program (1)
- Dental Plan (1)
- Diocesan Fiscal Management Conference (1)
- ERISA (1)
- Education (1)
- Emergency Contacts (1)
- Evidence of Insurability (EOI) (1)
- Fair Labor Standards Act (1)
- Health Savings Accounts (1)
- IRS Form 1094-B/C (1)
- IRS Form 1095-B (1)
- IRS Form 1095-B/C (1)
- IRS Guidance on Disaster Recovery (1)
- IRS Revenue Procedure 2023-29 (1)
- Life Insurance Benefits (1)
- Nondiscrimination Testing (1)
- OFCCP (1)
- Office of Civil Rights (OCR) (1)
- Personal Data (1)
- Pregnant Workers Fairness Act (PWFA) (1)
- Rehabilitation Act (1)
- Religous & Nonprofit Practice (1)
- Securities and Exchange Commission (SEC) (1)
- Single Sign On (SSO) (1)
- Training (1)
- Tuition (1)
- Voluntary Self-Identification of Disability Form (1)
- economic impact payment (1)
- unemployment resource (1)
Blog Archive
- June 2025 (8)
- May 2025 (20)
- April 2025 (20)
- March 2025 (20)
- February 2025 (20)
- January 2025 (25)
- December 2024 (15)
- November 2024 (15)
- October 2024 (20)
- September 2024 (20)
- August 2024 (25)
- July 2024 (15)
- June 2024 (20)
- May 2024 (25)
- April 2024 (20)
- March 2024 (20)
- February 2024 (25)
- January 2024 (20)
- December 2023 (15)
- November 2023 (21)
- October 2023 (20)
- September 2023 (20)
- August 2023 (25)
- July 2023 (15)
- June 2023 (25)
- May 2023 (20)
- April 2023 (20)
- March 2023 (25)
- February 2023 (20)
- January 2023 (20)
- December 2022 (15)
- November 2022 (15)
- October 2022 (20)
- September 2022 (20)
- August 2022 (21)
- July 2022 (15)
- June 2022 (20)
- May 2022 (20)
- April 2022 (20)
- March 2022 (25)
- February 2022 (20)
- January 2022 (20)
- December 2021 (20)
- November 2021 (15)
- October 2021 (20)
- September 2021 (25)
- August 2021 (20)
- July 2021 (25)
- June 2021 (20)
- May 2021 (20)
- April 2021 (25)
- March 2021 (20)
- February 2021 (20)
- January 2021 (20)
- December 2020 (16)
- November 2020 (15)
- October 2020 (25)
- September 2020 (20)
- August 2020 (20)
- July 2020 (29)
- June 2020 (20)
- May 2020 (20)
- April 2020 (25)
- March 2020 (22)
- February 2020 (15)
- January 2020 (25)
- December 2019 (15)
- November 2019 (15)
- October 2019 (25)
- September 2019 (20)
- August 2019 (25)
- July 2019 (15)
- June 2019 (20)
- May 2019 (20)
- April 2019 (20)
- March 2019 (20)
- February 2019 (22)
- January 2019 (25)
- December 2018 (15)
- November 2018 (19)
- October 2018 (17)
- September 2018 (20)
- August 2018 (16)
- July 2018 (14)
- June 2018 (19)
- May 2018 (23)
- April 2018 (20)
- March 2018 (25)
- February 2018 (20)
- January 2018 (20)
- December 2017 (16)
- November 2017 (20)
- October 2017 (20)
- September 2017 (20)
- August 2017 (25)
- July 2017 (20)
- June 2017 (25)
- May 2017 (20)
- April 2017 (21)
- March 2017 (25)
- February 2017 (20)
- January 2017 (20)
- December 2016 (21)
- November 2016 (15)
- October 2016 (20)
- September 2016 (25)
- August 2016 (20)
- July 2016 (20)
- June 2016 (25)
- May 2016 (20)
- April 2016 (20)
- March 2016 (20)
- February 2016 (20)
- January 2016 (21)
- December 2015 (15)
- November 2015 (15)
- October 2015 (26)
- September 2015 (19)
- August 2015 (20)
- July 2015 (25)
- June 2015 (20)
- May 2015 (20)
- April 2015 (25)
- March 2015 (19)
- February 2015 (19)
- January 2015 (20)
- December 2014 (15)
- November 2014 (15)
- October 2014 (25)
- September 2014 (20)
- August 2014 (19)
- July 2014 (22)
- June 2014 (19)
- May 2014 (25)
- April 2014 (24)
- March 2014 (22)
- February 2014 (27)
- January 2014 (25)
- December 2013 (23)
- November 2013 (16)
- October 2013 (26)
- September 2013 (20)
- August 2013 (26)
- July 2013 (20)
- June 2013 (24)
- May 2013 (32)
- April 2013 (26)
- March 2013 (28)
- February 2013 (26)
- January 2013 (35)
- December 2012 (22)
- November 2012 (27)
- October 2012 (28)
- September 2012 (26)
- August 2012 (33)
- July 2012 (26)
- June 2012 (29)
- May 2012 (42)
- April 2012 (36)
- March 2012 (37)
- February 2012 (26)
- January 2012 (22)
- December 2011 (8)
- November 2011 (7)
- October 2011 (5)
- September 2011 (14)
- August 2011 (12)